The CWU has regularly issued advice to its Branches, highlighting the serious illness which can be contracted as a result of being bitten by a tick; and this website has featured the issue and publicised the information in the LTBs.
 It is a mistaken common belief that only few areas of human activity place people at risk of being bitten by a tick carrying the bacteria and is confined to only those working in woodlands and farms. Reading the list of those at risk of the disease is quite sobering, because they fall into one of two groups.
It is a mistaken common belief that only few areas of human activity place people at risk of being bitten by a tick carrying the bacteria and is confined to only those working in woodlands and farms. Reading the list of those at risk of the disease is quite sobering, because they fall into one of two groups.
So Who is at risk of acquiring Lyme disease?
* Occupational: Forestry workers, deer managers, gamekeepers,
farmers, soldiers, outdoor educators, conservationists.
* Recreational: ramblers, campers, ornithologists, nature
photographers, returning travelers (from focal regions in US and
EU) disease.
But whilst the risk of being bitten by a tick is presumed to always be around the ‘summer’ months, evidence is now growing around the world that the true size of the problem is well underestimated, as diagnosis of the disease most commonly associated with a tick bite, is going undetected and untreated. This has devastating consequences for those suffering from Lyme Disease.
This is how one US based website describes the affect on those suffering from the disease:
“Unrelenting pain. Headaches, muscle aches, swollen joints, rashes. Loss of coordination and muscle spasms. Intermittent paralysis. Cycles of disabling symptoms that persist for years, causing ceaseless suffering and frustration for patients and their families.”
The website goes on to report on the disease describing it as “…..one of the most serious and controversial epidemics of our time.”
 Sonia Poulton, a freelance journalist who writes features for the Daily Mail on-line commented about the disease on her Facebook page over the weekend saying:
Sonia Poulton, a freelance journalist who writes features for the Daily Mail on-line commented about the disease on her Facebook page over the weekend saying:
“Heartbreaking. Lyme Disease is another, apparently, invisible illness. It has devastating consequences for the carrier. Sadly, as with ME and Fibro and much of mental health, it's left to those who are most ill to keep campaigning for awareness.
Those in power - including Govt. and Media - have neither the desire or know-how to do anything constructive. It's another injustice. One of many. And each and every one of them needs to be picked off until people are given the care they need.”
One respondent to Sonia's comment is that of a prolific blogger who goes by the name of Lymeywifey. Advising she had contracted Lyme Disease in 2008, she wrote:
"I have had no proper NHS treatment in all that time. I had to crawl to bed last night. It affects my ability to walk, amongst other things. I am one of the lucky ones- I am able to afford private treatment. It is a treatable disease, even in its chronic form, long term antibiotics usually produce great improvements and sometimes complete remission.
However the NHS continues to deny chronic Lyme patients this treatment and so thousands are suffering the devastating consequences. It is a disease only the relatively affluent can recover from. Its also much more common than official statistics suggest as it is massively under diagnosed."
Her blog offers practical advice and information about her experience of the disease.
The website of one Dr Merco, a US physician, promotes a documentary about the disease, entitled “Under Our Skins” and comments on the state of the US system of healthcare provision in tackling the disease:
“Each year, thousands go undiagnosed or misdiagnosed, often told their symptoms are all in their heads.”Under Our Skin" brings into focus a troubling picture of a health care system that is far too willing to put profits ahead of patients. The Chicago Daily Herald calls it "a ripping indictment of the medical establishment's failure to uphold its oath."
 Whilst in the UK, little concern seems to be evident within the Dept of Health, The Republic of Ireland; is taking a totally different stance with research on the disease and its causes and cures, continuing.
Whilst in the UK, little concern seems to be evident within the Dept of Health, The Republic of Ireland; is taking a totally different stance with research on the disease and its causes and cures, continuing.
According to this month's (Oct 2012) Irish Medical Journal, Lyme disease is a multi-system infectious disease caused by the Borrelia spirochaete genus. The predominant species in North America is Borrelia burgdorferi sensu stricto, and in Europe the predominant species are B. afzelli and B. garinii.
Lyme disease is the most frequently reported arthropod–borne infection of the nervous system both in Europe and the USA.
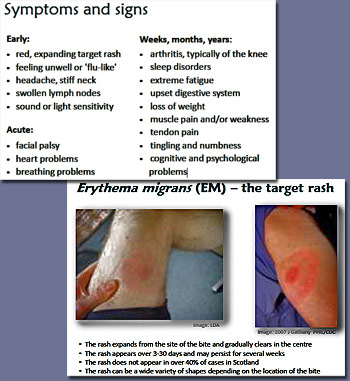
Erythema migrans (EM), the rash often seen in the early stage of Lyme disease is regarded as the most common clinical marker of infection and is estimated to occur in 60-80% of patients.
It usually appears 7-10 days (range 1-33 days) after a tick bite, and takes the form of either a single expanding red patch, or a central spot surrounded by clear skin that is in turn ringed by an expanding red rash (looks like a bull's-eye) centred on the tick bite itself.
Neurological manifestations of Lyme disease (neuroborreliosis; NB) comprise an array of both central and peripheral neurological syndromes, mimicking a variety of common disorders.
These include meningitis, cranial neuropathies (with a predilection for the facial nerve), myeloradiculitis and mononeuritis multiplex.
 Studies report the Republic of Ireland as having one of the highest rates of Lyme disease in Europe, with the disease considered as endemic in the West of Ireland.
Studies report the Republic of Ireland as having one of the highest rates of Lyme disease in Europe, with the disease considered as endemic in the West of Ireland.
The NHS website NHS Choices says that Lyme Disease is a very difficult disease to diagnose due to how it presents as very similar to other health conditions:
“Lyme disease can be a difficult condition to diagnose, particularly in its latter stages. This is because its symptoms are also shared by other, more common conditions such as infections and arthritis. Blood tests are important and useful in acute infection but don’t always confirm the diagnosis."
The characteristic pink or red "bull’s-eye" rash of Lyme disease can provide an important clue, but only around 50% of people with the condition will develop the rash in the first three to 30 days.
If the victim does not develop a rash but develops flu-like symptoms followed by mid-late stage Lyme disease symptoms such as arthritis (joint pain and swelling), headaches and/or depression, their GP may ask whether they have spent time in woodland or heath areas where ticks are known to live.
The two major tests that are used to help diagnose Lyme disease are:
- enzyme-linked immunosorbent assay (ELISA) test
- Western Blot test
The first test that is undertaken is a type of blood test known as an enzyme-linked immunosorbent assay (ELISA) test. The ELISA test looks for specific antibodies that are produced by your immune system to kill the Borrelia burgdorferi bacteria.
The ELISA test is not 100% accurate as it can sometimes produce a positive result even when a person is not infected with Lyme disease (known as a false-positive result). This may happen if a different condition is causing the symptoms, such as syphilis, glandular fever or rheumatoid arthritis. Therefore, a positive ELISA test is followed by a further test known as the Western Blot test.
The Western Blot test involves taking a small blood sample. The proteins in the blood are separated using a process called gel electrophoresis and are then placed on a membrane (a thin sheet of permeable material). The proteins can then be studied for antibodies (used by the immune system) that are used to fight the bacteria Borrelia burgdorferi which causes Lyme disease.
However, there is no 100 % effective test for tick borne diseases, and so in the end a clinical diagnosis has to be made.
Further, the manufacturers of both the ELISA and Western Blot tests state that a negative result should NOT be taken as meaning you don't have Lyme Disease; but too many GPs are doing just that – presuming a negative result means the patient does not have the disease.
It seems that too much reliance is being placed upon the clinical tests which are not reliable, rather than on what the patient tells them and the evidence from a physical examination. Even in cases of the tell-tale rash being present, the test results seem to over-ride the physician’s examination of the patient.
 But according to the Lyme Disease Action website the problems as to why Lyme Disease is largely going unnoticed are four-fold:
But according to the Lyme Disease Action website the problems as to why Lyme Disease is largely going unnoticed are four-fold:
The Public is often unaware that ticks can carry disease. Patients may ignore a rash and being unaware of the significance of some symptoms, do not relate them to their GP. Thus easily diagnosed early Lyme disease can become very difficult-to-diagnose late and chronic Lyme disease.
Doctors often believe that Lyme does not exist in their area, they do not recognise the rash and they are unaware of the wide variation of symptoms that can affect almost every part of the body.
The Department of Health is guided by the Health Protection Agency and believes that awareness and diagnostic capability amongst doctors is adequate.
The Health Protection Agency (HPA) believes that Lyme disease is rare, easily curable if caught early and readily diagnosed by their tests. The HPA also believes that chronic Lyme disease does NOT exist!
Another victim's experience of the disease and lack of medical action, exemplifies a typical response.
Commenting in September 2011, at the end of an NHS Choices website article on Lyme Disease, Cazzh, a sufferer of the disease who was not correctly diagnosed tells a too often repeated experience of GP and even consultants attitude toward the disease:
“Six months prior to being diagnosed with Chronic Fatigue Syndrome, I had the typical bullseye rash (have photos to prove!) and my symptoms all kicked in starting with a stiff neck, unexplained fatigue and muscle & joint aches as well as occasional blurring vision etc.
I did not realise what the rash had been (I got it after walking in deer inhabited woodlands locally) and so accepted the 'dustbin diagnosis' of CFS. When I did realise, I had to change GP to find one who would listen and who then referred me to an Infectious Diseases Consultant after being tested for Lyme Disease. (which of course came back negative!)
He then tried to tell me that I had not got it despite the fact that I had had the rash with all the symptoms starting after it, because the test was negative! He also tried to tell me that Nottinghamshire is not known to have Lyme Disease! Err excuse me? I had to laugh!
So here I am, still with NO treatment and possibly harbouring an infection which could get worse, which could cause me to have all sorts of problems in the future! I cannot work, I cannot socialise like I used to and as for exercise, that is VERY limited! Thanks very much - not!
It is time that a better test was used and it is also time that NHS staff were educated much more thoroughly in this dreadful disease as at the moment, many more like me are being left untreated and uncared for where possibly Lyme Disease is concerned!”
 The tragedy is that localised or early Lyme disease generally responds well to appropriate antibiotics.
The tragedy is that localised or early Lyme disease generally responds well to appropriate antibiotics.
A full cure is usually achieved if the disease is diagnosed and treated promptly, but the cure rate decreases the longer treatment is delayed.
But with the current Tory-led government in the process of privatising the NHS and the likes of Virgincare and Circle Health taking over the running of NHS hospitals for profit e.g. Hitchinbrooke NHS Trust hospital in Cambridgeshire by Circle Health; it is clear that the demand for profit will determine exactly where medical priorities will be, I.E. with the most common and profitable health conditions to treat.
So, just where are the 'risk hot-spots' of being bitten by a tick and developing Lyme Disease in the UK?
* New Forest, Thetford Forest, South Downs, Exmoor,
woodland/heathland in southern England, North York Moors,
Lake District, Scottish Highlands
* Other local areas (habitat - host species - humans)
* Therefore, important to note, infected ticks can be found in
both rural and urban green space – forests, parks, gardens.
Finally, the Lyme Disease Action website says that more research in the UK is required simply because:
Clinicians need guidance, and guidance should be based on evidence of what works and what fails to work.
Patients need to know the benefits, the side effects and the drawbacks of treatment so they can make informed decisions.
Further, they warn that :
As things stand, there is insufficient evidence on which to base treatment guidelines.
As a first stage in providing evidence based guidelines, LDA is funding a process to document the uncertainties in diagnosis and treatment of Lyme disease. The current situation leaves sufferers with permanent physical and mental health damage, and the lack of action by those agencies who should be ensuring public health is an indictment upon the Dept of Health, The Health Protection Agency, the UK Government and the NHS itself.
See also:
Early Warning Of The Risk Of Tick Bites As Weather Becomes Warmer (first published March 2012)
The Neglect Of Lyme Disease Patients And Horrors Of The Disease
Further information can be obtained from the E-Library Database here
Watch videos of a lecture given in Leicester about Lyme Disease, its diagnosis and treatment here
The feature length film 'Under Your Skin' can also be viewed or downloaded here
Web links for further information:
Lymeywifey - a blog from a Lyme Disease sufferer can be accessed here
Borreliosis and Associated Diseases Awareness UK - here
Lyme Disease Action - here
Source: Irish Medical Journal / NHS Choices / DermNet NZ / Dr Mercola website / Sonia Poulton / CWU / Lyme Disease Action

